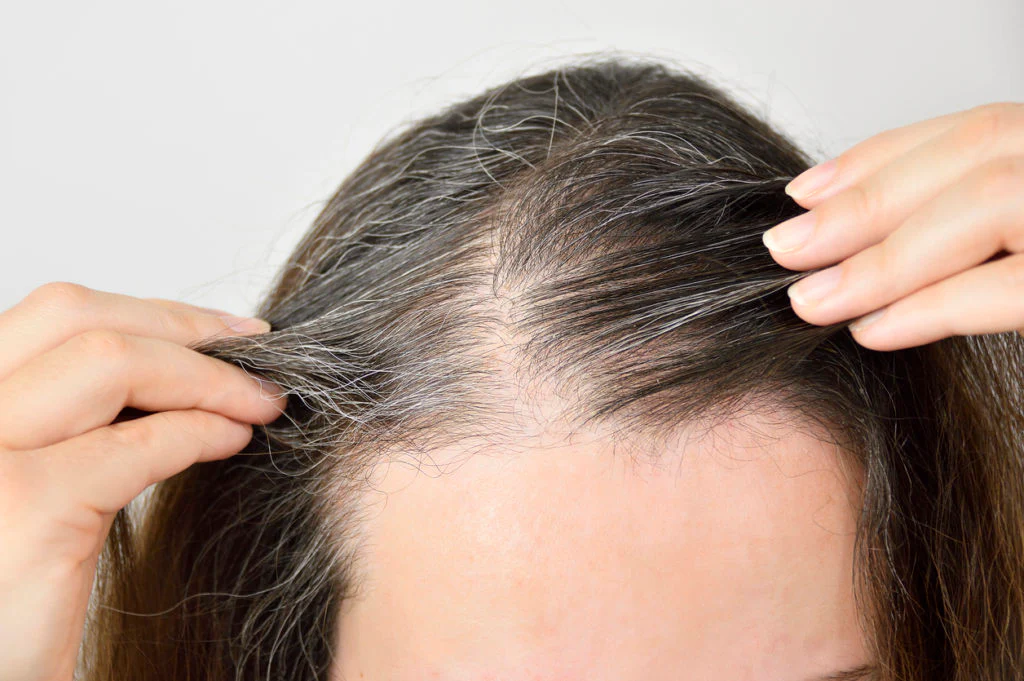
At Kopelman Hair, distinguishing between temporary shedding and progressive baldness is a key part of diagnosis. Dr. Kopelman evaluates patterns, timing, and underlying triggers to determine whether the condition is reversible or requires long-term management.
This approach helps guide the most effective treatment plan for each case.
Key Takeaways
- Telogen effluvium is short-term shedding triggered by stress, illness, or hormones. Androgenetic alopecia usually causes lasting thinning.
- Temporary hair shedding happens suddenly and improves in months. Pattern baldness, including female pattern hair loss, develops slowly and does not stop on its own.
- Both conditions can overlap. Treatment ranges from supportive care to medical therapy or surgery.
- Shedding in women often appears after childbirth or menopause. In men, genetics play a major role.
- Consulting a specialist like Dr. Kopelman provides clear answers, support, and long-term results.
Quick Comparison
Telogen Effluvium vs Androgenetic Alopecia Differences
Before exploring each condition in depth, this table summarizes the most important differences at a glance.
What Is Telogen Effluvium?
Is a short-term form of hair shedding. It happens when many follicles enter the resting phase of the growth cycle, called the telogen phase. Shedding often starts a few months after a major trigger, and patients notice a sudden drop in density.
To understand why this matters, it helps to know how the growth cycle works. Each strand cycles through four stages: anagen (active growth lasting 2 to 7 years), catagen (a brief two-week transition), telogen (a resting period of about three months), and exogen (the natural release of the strand).
In a healthy scalp, roughly 85 percent of follicles are in the anagen phase and only 10 to 15 percent are resting. During an episode of temporary hair shedding, that resting percentage can spike to 30 percent or more, pushing far more strands toward release at once.
Patient scenarios
Many women experience this kind of shedding after childbirth, often around three months postpartum, when estrogen levels drop sharply. Others lose noticeable amounts of hair after a high fever, COVID infection, surgery, or rapid weight loss.
Patients sometimes describe finding clumps in the shower drain or on the pillow each morning. These cases all share one thing in common: a clear triggering event followed by sudden, even thinning across the scalp.
Causes and triggers
The common causes of hair loss include fever, childbirth, rapid weight loss, poor diet, iron or vitamin D deficiency, thyroid imbalance, and certain medications such as beta-blockers, anticonvulsants, retinoids, and some antidepressants.
Major emotional stress, like grief or trauma, can also push more follicles into the resting stage at once. Crash diets and protein deficiency are common but often overlooked culprits. For a deeper look at other triggers, see our article on what causes hair loss.
When the trigger persists for more than six months, the condition becomes chronic, often linked to ongoing thyroid issues, autoimmune conditions, or long-standing nutritional gaps.
How many hairs fall in a temporary shedding condition?
The normal number of strands lost daily is 50 to 100. During a shedding episode, people may lose 300 or more, sometimes pulling out 5 to 10 hairs with a gentle tug. This is easily visible on pillows, in the shower, or on a brush.
How long does hair loss last?
Most cases last three to six months, with full recovery typically taking 6 to 9 months once the trigger is addressed. Hair usually grows back at its normal rate of about half an inch per month, though density may take a year or longer to fully restore.
What Is Androgenetic Alopecia?
Androgenetic alopecia, also known as pattern baldness, is a chronic and progressive condition. Unlike the temporary form of shedding, it does not stop naturally and tends to worsen over time without intervention.
The role of DHT and follicle miniaturization
This condition is driven by sensitivity to dihydrotestosterone, or DHT, a hormone derived from testosterone. DHT binds to androgen receptors on genetically susceptible follicles and gradually shortens their growth phase.
Each cycle, the follicle produces a slightly thinner, shorter strand. This process is called follicular miniaturization, and over years it transforms thick terminal hairs into fine vellus hairs that barely break the surface of the skin.
Eventually, affected follicles can stop producing visible strands altogether, though the follicle itself often remains alive for some time before becoming dormant.
Causes and risk factors
Family history is the strongest predictor. If close relatives on either side of the family experienced pattern baldness, the risk is significantly higher. Age plays a role too: roughly 50 percent of men show signs by age 50, and up to 80 percent are affected by age 70.
In women, hormonal changes around menopause and conditions like polycystic ovary syndrome can accelerate the process. Ethnicity also matters, with Caucasian men typically affected earliest and most severely.
Symptoms and progression
Men often see receding hairlines (classified on the Norwood scale, from stages I to VII) starting at the temples, followed by thinning at the crown. The two areas can eventually meet, leaving a horseshoe-shaped band of hair around the sides and back.
Women notice female pattern hair loss as a widening part line and diffuse thinning over the top of the scalp, classified using the Ludwig scale (stages I to III). The frontal hairline is usually preserved, which helps distinguish it from other female-specific causes of thinning.
Diagnosis methods
Doctors check the scalp visually, review family history, and use trichoscopy, a magnified examination that reveals miniaturized follicles, varying hair shaft diameters, and yellow dots. They may also order blood tests to rule out thyroid disease, iron deficiency, or hormonal imbalance.
In unclear cases, a small scalp biopsy can confirm the diagnosis by showing the ratio of terminal to vellus hairs. A T:V ratio below 4:1 strongly suggests pattern baldness, while telogen percentages above 15 percent on biopsy point to the temporary, stress-related form.
Key Differences Between Telogen Effluvium and Alopecia
People often ask about androgenetic alopecia vs telogen effluvium. The two can look alike in early stages, but they differ in cause, course, and treatment response.
How to tell the difference?
Temporary hair shedding starts suddenly and causes diffuse shedding evenly across the scalp. Pattern baldness develops slowly in a clear, recognizable shape, either receding hairlines and crown loss in men or part widening in women.
A simple at-home check: look at old photos from one to two years ago. Sudden, dramatic change after a stressor points to the temporary form, while gradual thinning that creeps up over years suggests the genetic kind.
Temporary hair shedding vs androgenetic alopecia symptoms
The symptoms differ in three key ways. First, timing: stress-related shedding hits suddenly and often resolves within months, while genetic thinning is slow and steady.
Second, distribution: the temporary type is even and all-over, with no specific pattern, while the hereditary form follows defined zones (temples, crown, or part line). Third, follicle health: under magnification, follicles look healthy in stress-related shedding but progressively miniaturized in pattern baldness.
Onset, duration, and pattern
Stress-related shedding improves in months once the trigger resolves. Genetic thinning gets worse over time and requires ongoing treatment to halt or reverse, with most patients seeing measurable change over 6 to 12 months of consistent therapy.
Temporary hair shedding vs androgenetic alopecia treatment
Stress-related episodes often improve on their own with rest, nutritional support, and time. Pattern baldness typically requires minoxidil, oral medications such as finasteride or dutasteride, low-level laser therapy, PRP, or surgical restoration to see lasting results.
In short, one form is sudden and temporary, while the other is gradual and long-lasting.
Telogen Effluvium vs Specific Types of Alopecia
Can telogen effluvium look like alopecia areata?
Yes, but the patterns differ clearly. Alopecia areata creates round, well-defined bald patches with smooth skin underneath, often appearing within days. Stress-related shedding causes even thinning across the entire scalp without bald spots.
Temporary hair shedding vs alopecia areata symptoms
Alopecia areata shows defined patches and may include the classic “exclamation mark” hairs (short, broken strands tapering near the root). It is also linked to autoimmune conditions like thyroiditis and vitiligo.
The temporary stress-related form is more diffuse, lacks visible bald patches, and is not autoimmune in nature.
Temporary hair shedding vs alopecia totalis
Alopecia totalis results in complete loss of scalp hair, including eyebrows and lashes in advanced cases. The stress-related form never progresses to total baldness and does not damage the follicles permanently.
Androgenetic Alopecia and Telogen Effluvium: Overlap and Coexistence
Shared symptoms and confusion
Both conditions can cause thinning, which often confuses patients and even some clinicians. The temporary form may also unmask hidden genetic thinning by clearing out resting hairs and exposing the underlying density loss patients had not yet noticed.
This is why some people feel their hair “never came back the same” after a stressful event, when in reality the genetic process was already underway.
When both occur together
Some patients have both conditions at once, especially women in midlife, postpartum mothers with family history of pattern baldness, and men under chronic stress with a hereditary predisposition. Doctors must determine which portion is temporary and which is permanent.
This often requires a combined approach: treating the underlying trigger while simultaneously starting long-term therapy for the genetic component to prevent further progression.
Temporary hair shedding vs Alopecia in Women and Men
Telogen effluvium vs androgenetic alopecia in women
Shedding in women often starts during pregnancy, postpartum, or perimenopause. Postpartum shedding peaks around three to four months after delivery and improves within 6 to 12 months.
Menopause can expose underlying female pattern hair loss as estrogen decline allows androgens to influence sensitive follicles more strongly. Iron deficiency, low ferritin, thyroid imbalance, and crash dieting are also common contributors in women.
Treatment in women may include topical minoxidil 5%, spironolactone, oral minoxidil at low doses, and addressing nutritional or hormonal triggers. You can also read about related concerns like a receding hairline in women.
Male-specific patterns and treatment
Men often notice receding hairlines and crown thinning starting in their 20s or 30s. Stress can layer telogen-phase shedding on top of genetic thinning, making changes appear faster and more dramatic than they actually are.
Common treatments for men include finasteride 1mg daily, topical or oral minoxidil, dutasteride for resistant cases, PRP injections, and follicular unit extraction (FUE) for permanent restoration.
Telogen Effluvium vs Alopecia Pictures
What pictures can show
Photos can help spot diffuse shedding versus pattern thinning. Doctors use standardized angles (top-down, front, sides, and part-line views) to track changes objectively over time.
For more examples, see our gallery of pictures of telogen effluvium.
When photos help diagnosis
At-home photos taken every three months under consistent lighting help patients and providers monitor progress. Doctors compare images side-by-side using digital trichoscopy software to measure hair density, shaft diameter, and follicle counts per square centimeter.
This method also helps confirm if both conditions are present, since one shows a sharp drop followed by recovery, while the other shows steady decline regardless of trigger.
Emotional and Psychological Impact
Hair loss affects more than appearance. Many people report stress, anxiety, social withdrawal, and reduced self-confidence. Studies show up to 50 percent of patients with hair thinning experience symptoms of depression or anxiety related to their condition.
Sudden shedding can feel alarming, especially when handfuls come out at once, while ongoing pattern thinning often produces a slow, grinding sense of loss. Both responses are valid and common.
Dr. Kopelman reminds patients that both conditions can be managed effectively. Talking with family, joining support groups, working with a therapist, or simply having a clear diagnosis often reduces anxiety considerably and makes treatment more effective.
Temporary hair shedding or Alopecia?
How can I tell if my shedding is a temporary shedding condition or alopecia?
Sudden, diffuse shedding within two to three months of a major life event, illness, or stressor strongly points to the temporary form. Slow, patterned thinning over years that follows family history points to the genetic type.
A clinical exam confirms the diagnosis through trichoscopy, a hair pull test (where 4 to 6 hairs are gently tugged; more than 10 percent shedding suggests active loss), and sometimes blood work or biopsy.
Treatment and Management Options
Medical treatments
For pattern baldness, FDA-approved options include topical minoxidil (2% or 5% solution or foam) and oral finasteride 1mg daily for men. Studies show that combining the two produces results in roughly 94 percent of men over 12 months, compared to 80 percent for finasteride alone and 59 percent for minoxidil alone.
Dutasteride, spironolactone (for women), and low-dose oral minoxidil are increasingly used as off-label options. PRP (platelet-rich plasma) and low-level laser therapy can be added to support density gains.
The temporary stress-related form often improves without long-term medication, though minoxidil may be used short-term to speed recovery in particularly dramatic cases.
Lifestyle and supportive care
Healthy eating, stress management, and gentle styling all help. Iron, ferritin, vitamin D, zinc, biotin, and protein intake should be checked and corrected if low, since deficiencies are a leading reversible cause.
Sleep quality, exercise, mindfulness, and reducing exposure to harsh heat tools, tight ponytails, and chemical treatments support recovery in both conditions.
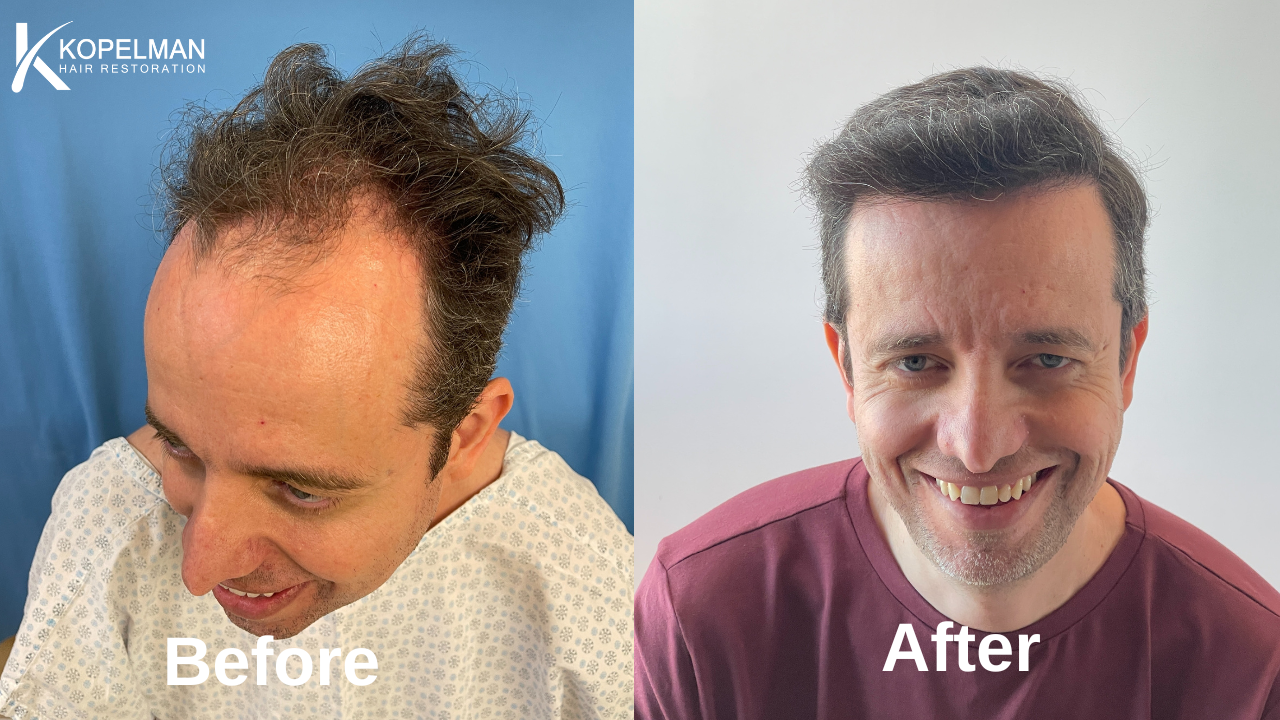
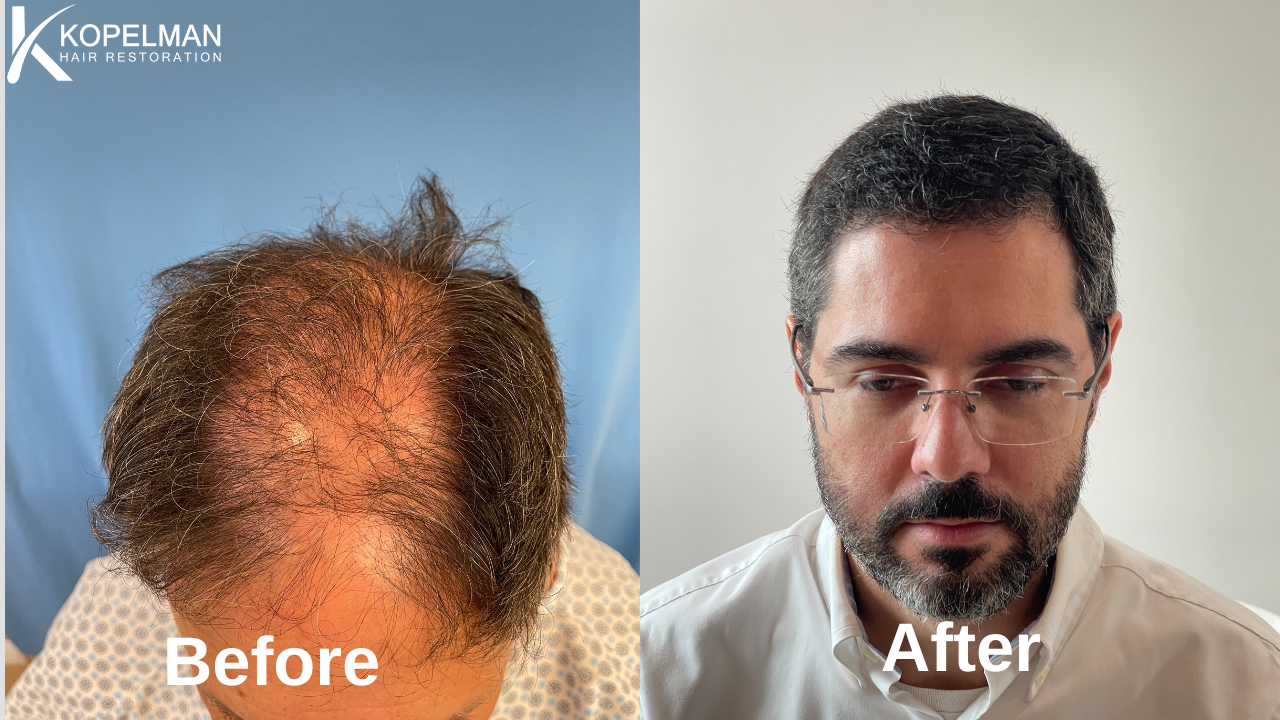
Advanced hair restoration
For permanent loss, FUE and FUT hair transplants offer durable, natural-looking results. Modern techniques can transplant 1,500 to 4,000 grafts in a single session, with costs typically ranging from $4,000 to $15,000 depending on graft count and clinic.
At Kopelman Hair, Dr. Kopelman uses advanced robotic and manual extraction methods to achieve dense, undetectable restoration in both men and women.
In short, the temporary form improves with time and supportive care, while the genetic kind requires consistent treatment to slow or reverse progression.
Prevention and Early Intervention
Early steps can lower risk and protect existing density:
- Eat a protein-rich, balanced diet with adequate iron, zinc, and vitamin D.
- Manage stress with regular exercise, sleep, and mindfulness practices.
- Avoid tight hairstyles, harsh chemical treatments, and excessive heat styling.
- Visit a doctor when shedding lasts longer than three months or worsens.
- Get blood work annually if you have a family history of thinning.
Patients with a family history should see a specialist regularly. Early diagnosis allows treatment to begin before significant miniaturization occurs, which typically produces the best long-term results.
When to Seek Professional Help
If shedding is heavy, persistent, accompanied by scalp itching or pain, or causing distress, schedule an evaluation. Dr. Kopelman and his team determine whether the cause is temporary, genetic, or a combination of both.
Early diagnosis leads to better outcomes, since starting treatment within the first 6 to 12 months of pattern baldness onset typically produces the most dramatic regrowth.
To get clear answers and explore personalized treatment options, schedule a consultation with Kopelman Hair today.