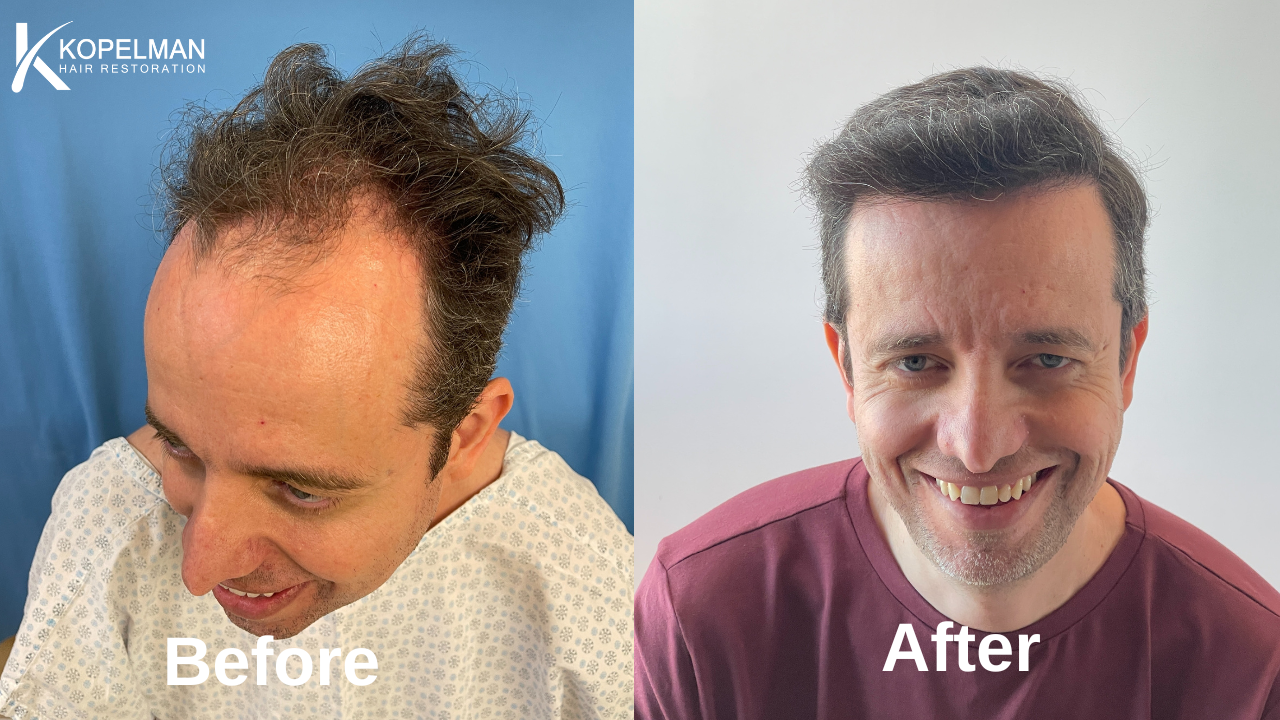
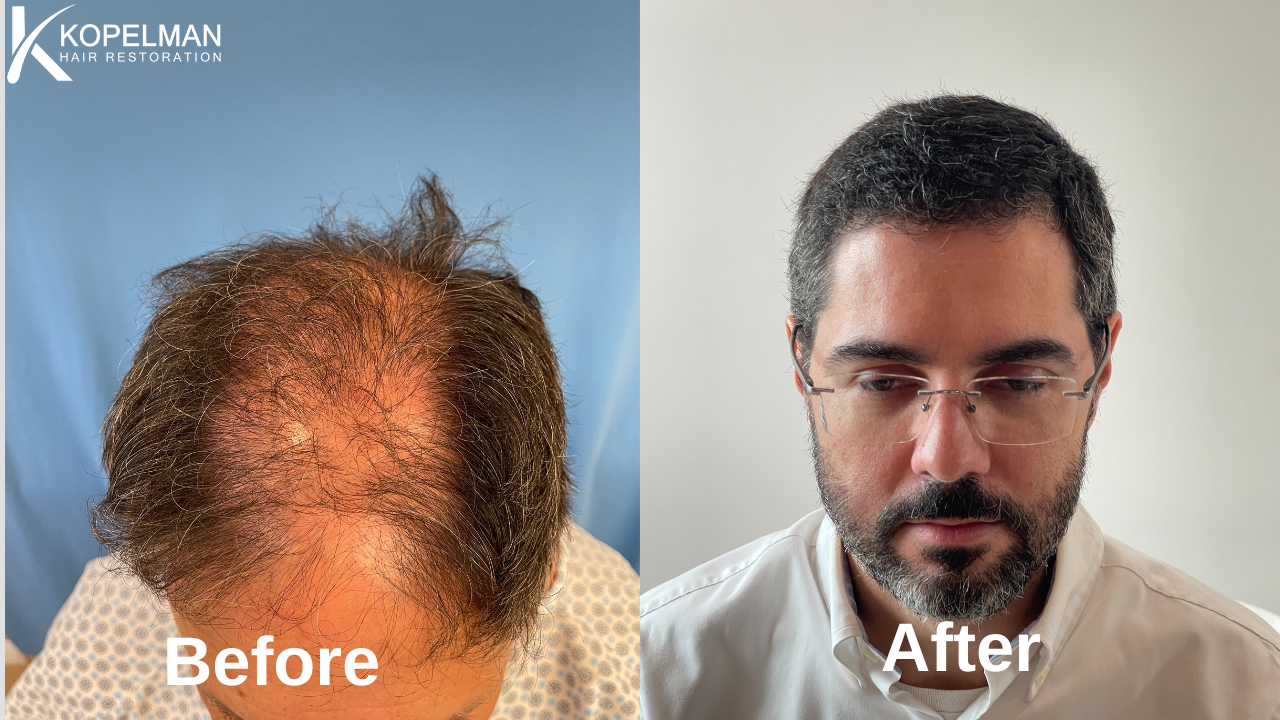
At Kopelman Hair, patients receive expert diagnosis and personalized treatment for follicle conditions caused by underlying medical issues. With over 40 years of experience, Dr. Ross Kopelman helps patients restore scalp health and confidence through advanced, medically guided care.
Key Takeaways
- Syphilis is the only sexually transmitted disease confirmed to directly cause shedding, presenting clinically as alopecia syphilitica.
- Alopecia syphilitica affects an estimated 3% to 7% of patients in the secondary stage, according to dermatology literature indexed on PubMed Central.
- HIV does not directly damage follicles, but immune stress, nutrient depletion, and certain medications can trigger diffuse thinning.
- In secondary syphilis, the condition often appears as patchy “moth-eaten” spots on the scalp, beard, or eyebrows.
- Some treatments for chlamydia and other infections, such as azithromycin, may indirectly contribute to shedding through nutrient depletion.
- Early diagnosis and proper antibiotic therapy can stop further follicle damage and support full regrowth within weeks to a few months.
Understanding the Link Between STDs and Hair Loss
Sexually transmitted infections affecting the scalp are uncommon, but well-documented in dermatology. These infections can disrupt how the body repairs and regenerates follicles. When untreated, certain pathogens damage the dermal papilla or interfere with hormones and nutrient delivery, leading to thinning.
Most common STDs, such as chlamydia, gonorrhea, or herpes, do not cause shedding directly. However, syphilis and HIV can alter the growth cycle by disturbing blood flow, immune function, or nutrient absorption. The U.S. Centers for Disease Control and Prevention has reported a steady rise in syphilis cases over recent years, making awareness of its dermatologic signs more important than ever.
Dr. Ross Kopelman emphasizes that the first step in managing this type of follicle damage is treating the infection, then restoring scalp and root health with a tailored care plan.
Which STDs Can Cause Hair Loss
People often ask, can STDs cause hair fall across the board, or only in specific cases? The answer is nuanced. Syphilis is the only confirmed direct cause, while others contribute indirectly through inflammation, treatment side effects, or nutritional depletion.
1. Syphilis
Syphilis is a bacterial infection caused by Treponema pallidum. It spreads through sexual contact and develops in stages if untreated. Shedding usually occurs during the secondary stage, weeks or months after initial infection.
Patients may develop the condition known clinically as alopecia syphilitica, which presents in three recognized patterns: a diffuse pattern of evenly thinned strands, the classic “moth-eaten” pattern of small irregular patches, or a combination of both. This happens when the bacteria infect skin and follicles, disrupting the growth cycle.
Trichoscopy, a non-invasive scalp imaging technique, often reveals characteristic findings in alopecia syphilitica. These include black dots, broken strands, yellow dots, and exclamation mark hairs, features that help dermatologists distinguish it from alopecia areata.
Other signs of secondary syphilis include:
- Painless rash on the body, palms, or soles
- Swollen lymph nodes or sore throat
- Fatigue, fever, and aching joints
- Painless sores following sexual activity
With prompt antibiotic treatment, syphilis-related shedding is reversible and regrowth typically begins within 5 weeks to 3 months, according to peer-reviewed evidence from dermatology journals.
2. HIV (Human Immunodeficiency Virus)
HIV weakens the immune system, making the body more vulnerable to secondary conditions that can cause shedding. The virus itself does not directly damage follicles, but immune stress, nutrient depletion, and antiretroviral (ART) side effects can contribute to thinning. Older HIV medications were known to cause shedding as a side effect, though most modern regimens have far fewer adverse effects.
Common signs include:
- Diffuse thinning across the scalp
- Slower regrowth and weakened strands
- Brittle or easily broken texture
- Dry or irritated scalp
Density often improves with stable HIV treatment, balanced nutrition, and gentle care. In persistent cases, platelet-rich plasma (PRP) or low-level laser therapy (LLLT) can help restore scalp circulation and stimulate new growth.
3. Other Infections and Indirect Contributors
Beyond syphilis and HIV, several other infections can play an indirect role. Pubic lice infestations, while not technically affecting the scalp, can cause inflammation and severe itching that leads to scratching, secondary bacterial infection, and temporary baldness in affected zones. Trichomoniasis, a parasitic infection, has occasionally been linked to localized irritation in body areas exposed to the pathogen.
Chlamydia and gonorrhea do not produce a direct STD on scalp tissue, but their treatment regimens sometimes affect follicle health. Azithromycin, a macrolide antibiotic commonly prescribed for chlamydia, can deplete vitamin B and hemoglobin levels in some patients, occasionally resulting in shedding.
How STDs Affect the Hair Growth Cycle
Each strand grows in three stages: anagen (growth), catagen (transition), and telogen (resting). Infections, inflammation, and stress can shift large numbers of follicles into the resting stage, causing noticeable shedding several weeks later.
- In syphilis, bacteria invade follicles and trigger an inflammatory immune response that disrupts the growth cycle.
- A second proposed mechanism involves a buildup of lymphocytes, a type of white blood cell, that plug the follicular opening.
- In HIV, immune weakness and medication effects slow regrowth.
- Chronic infection also triggers inflammation that restricts scalp blood flow.
Treatment can also temporarily worsen the issue. The Jarisch-Herxheimer reaction (JHR) is an uncommon but well-documented side effect that occurs within the first 24 hours of antibiotic therapy for syphilis, sometimes producing transient shedding alongside fever, chills, and joint pain.
Early Signs That STD-Related Hair Loss May Be Occurring
Spotting symptoms early prevents long-term thinning or scarring. Watch for:
- Patchy bald spots or moth-eaten zones on the scalp, beard, or brows
- Diffuse shedding without an obvious genetic or hormonal cause
- A non-itchy rash, fever, or fatigue alongside scalp changes
- Persistent shedding despite consistent care
If these signs appear after possible STD exposure, seek both medical and dermatologic evaluation. Testing confirms whether infection or another condition is responsible.
How Doctors Diagnose STD-Related Balding
Diagnosis involves teamwork between a dermatologist and an infectious disease specialist. Accurate identification matters because the treatment pathway differs entirely depending on the underlying cause.
Steps may include:
- Medical History: Review of recent infections, medication use, sexual history, and immune health.
- Physical Exam: Assessment of scalp, beard, and brow patterns of thinning.
- Blood Tests: Antibody serology for syphilis (RPR or VDRL with treponemal confirmation), HIV screening, thyroid panel, and nutrient levels.
- Advanced Diagnostics: Trichoscopy, immunohistochemistry, or polymerase chain reaction (PCR) testing where indicated.
At Kopelman Hair, advanced imaging and scalp evaluation identify whether the underlying cause is infection, hormonal imbalance, or another factor, ensuring patients receive accurate and targeted care.
Treatment for STD-Related Hair Loss
1. Medical Treatment
The first step is treating the infection. According to guidance from the CDC syphilis pocket guide, the first-line therapy for syphilis is an injection of benzathine penicillin G, which clears the bacteria and allows regrowth typically within 5 weeks to 3 months.
For patients with a known penicillin allergy, doctors may prescribe oral doxycycline (Vibramycin-D, Periostat) or tetracycline (Sumycin, Achromycin V) as evidence-based alternatives. HIV is managed through antiretroviral therapy (ART), which controls the virus, restores immune function, and reduces shedding over time. Patients should always follow medical advice closely and avoid self-treatment, which can delay recovery.
2. Restorative Therapies
After infection control, scalp health can be supported with medical or minimally invasive options:
- Topical Minoxidil to boost blood flow and stimulate dormant follicles.
- PRP Therapy to deliver growth factors that encourage regrowth.
- LLLT to enhance circulation and support follicular activity.
- Nutritional Support with biotin, zinc, vitamin B complex, and vitamin D to reinforce strand strength.
3. Hair Transplant Surgery
For lasting or advanced thinning, transplantation provides permanent restoration. The procedure relocates healthy follicles to thinning zones for natural density. Dr. Kopelman recommends surgery only after infection resolution, immune stabilization, and a confirmed period of remission.
Can STD-Related Hair Loss Be Reversed?
Most cases are temporary when treated early. Once the infection clears and the scalp environment normalizes, regrowth typically begins within 5 weeks to 3 months, with full recovery often complete by six months.
Permanent loss may occur if:
- The infection remains untreated for long periods.
- Scarring develops in the affected zones.
- The patient also has genetic (androgenetic) thinning superimposed on the infection.
Early diagnosis and continued scalp care improve recovery outcomes significantly.
Other Conditions That Mimic STDs That Cause Hair Loss
Several conditions resemble infection-related shedding and must be ruled out for accurate diagnosis:
- Telogen Effluvium: Temporary shedding triggered by stress, illness, or surgery.
- Alopecia Areata: An autoimmune condition causing round patches of baldness.
- Tinea Capitis: A fungal scalp infection that can mimic moth-eaten patterns.
- Seborrheic Dermatitis: Scalp inflammation that weakens follicles.
- Androgenetic Alopecia: Genetic thinning in men and women.
Proper testing distinguishes these from infection-driven causes and guides appropriate treatment.
Prevention and Self-Care Tips
You can reduce your risk and support healthy follicles by:
- Practicing safe sex and getting tested regularly through a primary care provider or sexual health clinic.
- Considering pre-exposure prophylaxis (PrEP) where appropriate to reduce HIV transmission risk.
- Seeking prompt medical care for any possible STD exposure.
- Eating a balanced diet rich in protein, iron, B vitamins, and zinc.
- Avoiding smoking, excess alcohol, and harsh scalp products.
These steps help protect both general health and scalp resilience.
Emotional and Psychological Impact
Shedding tied to a sexually transmitted infection can feel especially distressing because it combines health concerns with social stigma. Many patients experience anxiety, embarrassment, or fear of permanent damage. At Kopelman Hair, treatment includes education, reassurance, and follow-up to support both emotional and physical recovery.
Discussing concerns openly with a trusted physician helps reduce the isolation patients sometimes feel. Recovery is the rule rather than the exception, and most patients regain full density once the infection is cleared.
When to See a Specialist
Schedule an appointment if:
- Shedding appears alongside other infection symptoms, such as a rash, fever, or sores.
- Thinning continues for more than three months after STD treatment.
- Bald patches do not improve within a few months of infection clearance.
- You notice a clinically significant STD on scalp area, such as moth-eaten patches or persistent inflammation.
Early care prevents permanent damage and restores healthy density faster.
Expert Insight From Dr. Ross Kopelman
In Dr. Kopelman’s clinical experience, infection-related shedding is one of the most reversible forms of follicle disruption he treats, provided patients seek care promptly. He notes that the moth-eaten pattern of alopecia syphilitica is often misdiagnosed as alopecia areata, which is why trichoscopy and serologic testing are essential before starting any restorative protocol.
He also reminds patients that regrowth timelines can vary based on infection duration, immune status, and concurrent conditions like genetic thinning. Most patients who complete antibiotic therapy see meaningful regrowth within 8 to 12 weeks. For those whose follicles do not fully recover, combination therapy involving PRP, laser stimulation, and nutrient support has produced consistent improvements in his practice.
His clinic emphasizes a comprehensive approach that addresses the medical, dermatologic, and psychological dimensions of recovery together, rather than in isolation.
Final Advice
Shedding linked to sexually transmitted diseases is uncommon but highly treatable. Syphilis remains the only infection that directly affects follicles, while HIV and certain medications can contribute indirectly. With early detection and professional treatment, most patients recover fully within a few months.
At Kopelman Hair, patients receive advanced, personalized care for all forms of follicle conditions. Whether caused by infection, hormones, or genetics, Dr. Kopelman and his team restore both density and confidence through safe, proven treatments backed by current dermatologic evidence.
Frequently Asked Questions
No, alopecia syphilitica is temporary in the vast majority of cases when the underlying infection is treated promptly with antibiotics. Regrowth typically begins within 5 weeks to 3 months after treatment.
Shedding generally resolves within 5 weeks to 3 months following antibiotic therapy, or until the infection progresses from the secondary to the latent stage if left untreated. The latent stage typically begins 1 to 2 years after initial exposure.
Syphilis is the only sexually transmitted infection known to directly cause shedding. However, treatments for HIV, gonorrhea, chlamydia, and herpes may produce temporary thinning as a medication side effect. Pubic lice infestations can also lead to localized hair loss through inflammation and scratching.
Chlamydia itself does not directly damage follicles. However, azithromycin, a common antibiotic used to treat it, can occasionally lead to thinning by depleting vitamin B and hemoglobin levels in some patients.
Doctors typically combine a medical and sexual history review, a physical exam of the scalp, blood antibody tests (RPR or VDRL with treponemal confirmation), and trichoscopy. PCR or immunohistochemistry tests may also be ordered when the diagnosis is uncertain.