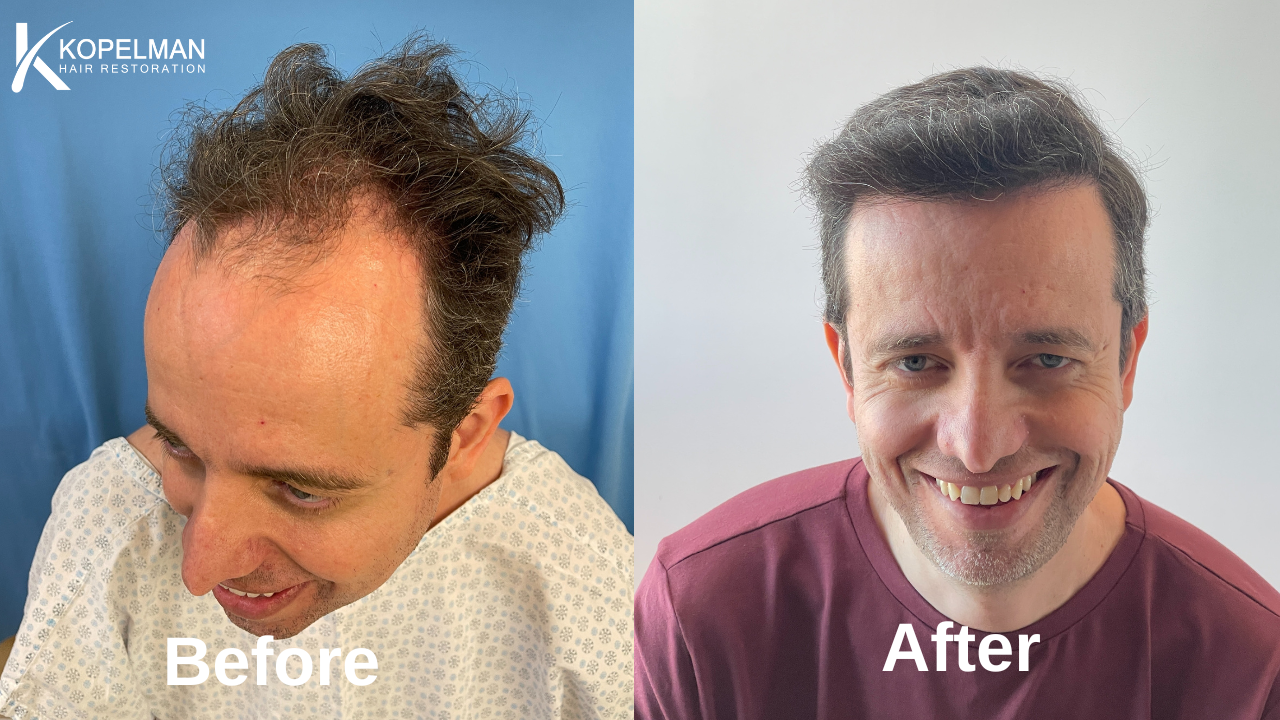
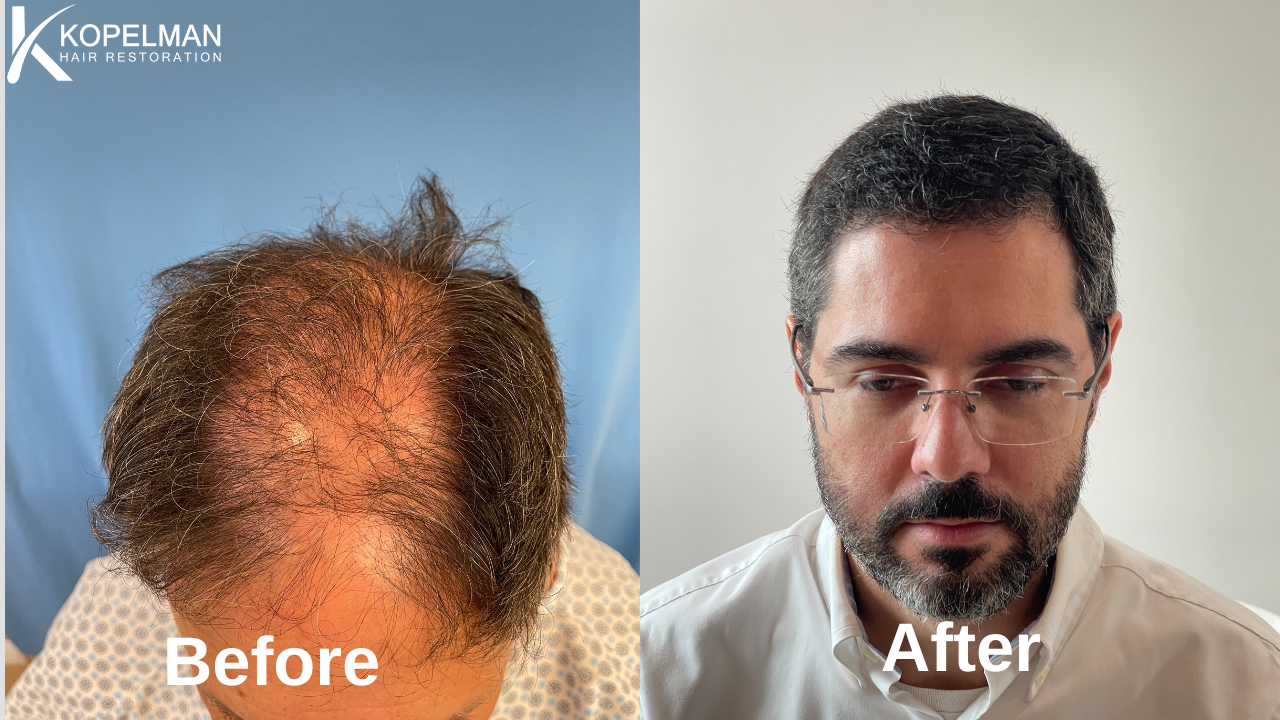
At Kopelman Hair, we often hear patients ask about the link between persistent scalp discomfort and shedding. While these symptoms may seem unrelated, they can share common biological pathways. Understanding the connection is key to finding effective solutions and protecting both your comfort and your hair.
Key Takeaways
- Headaches and hair loss can occur together due to stress, inflammation, autoimmune conditions, hormonal shifts, or rare disorders like cephalgia alopecia.
- Tracking patterns such as scalp sensitivity before shedding, or thinning that follows migraine episodes, can help identify the underlying cause.
- Medical evaluation may include scalp examination, bloodwork, autoimmune screening, and in some cases infectious disease testing such as RPR for syphilis.
- Treatment options depend on the cause and may involve stress management, medicated shampoos, OnabotulinumtoxinA injections, or specialist-led therapies.
What Causes Headaches and Hair Loss?
Headaches and shedding can happen at the same time due to shared triggers like stress, hormonal changes, scalp inflammation, or nerve dysregulation. These issues can disrupt both scalp comfort and follicle function, sometimes through overlapping biological pathways.
Stress, Hormones, and Lifestyle Factors
Stress is a common driver of tension headaches and sudden shedding. It raises cortisol levels, affects sleep, and can push follicles into a resting phase. This leads to telogen effluvium, a form of temporary diffuse thinning.
Hormonal shifts during postpartum, menopause, or thyroid dysfunction may also produce both symptoms. A healthy lifestyle can reduce flare-ups and support recovery.
Factors that contribute include:
- Poor sleep
- Nutritional deficiencies, particularly vitamin D, B vitamins, zinc, and omega-3 fatty acids
- Dehydration
- Overuse of caffeine or stimulants
Stress management and consistent routines may ease discomfort and protect follicle health.
Scalp Inflammation and Tenderness
Conditions like folliculitis or seborrheic dermatitis can cause localized soreness and shedding. These are often tied to inflammation that weakens follicles at the root.
Symptoms include:
- Tenderness when touching the scalp
- Flaking or redness
- Itching followed by shedding
Irritation from tight hairstyles, harsh products, or chemical treatments can worsen these effects. If discomfort includes both tightness and shedding, professional evaluation is often needed.
The Neurological Connection: How Migraines Can Affect Follicles
Brain-related conditions do not directly destroy follicles, but they can activate nerve pathways that disrupt the growth cycle. A 2020 peer-reviewed study by Drs. Kate Bedrin and Carrie Dougherty of Georgetown University Hospital, published in Current Pain and Headache Reports, provides the clearest explanation of how this happens.
Their research proposes that recurrent headaches trigger repeated activation of the trigeminal and upper cervical nerve branches, which run through the scalp and supply the follicles.
This repetitive signaling depletes two neuropeptides, substance P and calcitonin gene-related peptide (CGRP), that are essential for maintaining the follicle’s growth phase and regulating immune activity at the root level.
When these molecules drop below the threshold needed to sustain the anagen phase, follicles shift prematurely into the resting phase and shedding follows, often in the exact area of the scalp where the pain is concentrated.
This mechanism answers one of the most common questions patients bring to our clinic: can migraines cause hair loss? Based on the current evidence, yes, particularly in patients with chronic or recurrent migraines that consistently affect the same region of the scalp.
The connection is not psychological or coincidental; it is rooted in how the nervous system and the follicle communicate.
Medications used to treat neurological conditions can also contribute independently. Certain antiepileptics and mood stabilizers list thinning as a documented side effect, separate from the headache mechanism itself.
Newer migraine-specific therapies, particularly CGRP inhibitors like erenumab and fremanezumab, are being actively studied for their downstream effects on follicle health, though no definitive conclusions have been established yet.
Always consult a specialist before adjusting any migraine medication based on follicle concerns.
Autoimmune Disorders That Affect Both Symptoms
Some autoimmune diseases affect both the scalp and the nervous system. Many patients ask, “can alopecia cause headaches?” The answer is that certain forms of alopecia, particularly those tied to systemic autoimmune disease, can co-occur with chronic head pain because the underlying immune dysfunction affects multiple body systems.
Examples include:
- Lupus: Triggers chronic head pain and patchy shedding
- Alopecia areata: Causes sudden bald patches and may co-occur with migraine in some patients
- Hashimoto’s thyroiditis: Can lead to migraines and diffuse thinning
- Multiple sclerosis: May cause ongoing pain and shedding episodes
These conditions involve the immune system mistakenly attacking healthy tissues, including follicles. Managing the autoimmune condition typically improves both symptoms together.
Infections and Less Common Causes
Infectious causes are sometimes overlooked but can be significant. A clinical case published in Mayo Clinic Proceedings described a 31-year-old woman with seven months of daily head pain and roughly 50 percent diffuse shedding, ultimately diagnosed with secondary syphilis and neurosyphilis.
Alopecia syphilitica appears in 4 to 12.5 percent of patients with secondary syphilis and presents as a moth-eaten or diffuse pattern of shedding. After treatment with intravenous penicillin G, both her headaches and shedding resolved within six weeks.
This case illustrates an important point. When chronic head pain and unexplained shedding appear together, infectious and systemic causes deserve consideration alongside the more common stress and hormonal explanations.
How to Tell If Headaches Are Causing Hair Shedding
Tracking symptom patterns can reveal whether the two are connected. You might notice:
- Shedding increases in the days following a headache episode
- The scalp becomes sensitive or tender to touch
- Hair falls more from the area where pressure or pain is felt
- Burning or stabbing sensations precede a patch of thinning
Some people specifically report headaches and hair shedding after stressful events or migraine attacks. Keeping a symptom journal that tracks pain location, intensity, and shedding patterns helps clinicians determine if the two are linked or coincidental.
Headaches and Hair Loss in Women: Why It Happens More Often
Women are disproportionately affected by both migraines and certain types of alopecia, which is why headaches and hair thinning in women is a particularly common search. Hormonal fluctuations across the menstrual cycle, pregnancy, postpartum, perimenopause, and menopause can drive both conditions.
Estrogen withdrawal after childbirth or during menopause is a known trigger for telogen effluvium and for migraines. Thyroid disorders, polycystic ovary syndrome, and iron deficiency are also more prevalent in women and contribute to both symptoms.
Autoimmune conditions, including lupus and Hashimoto’s thyroiditis, are far more common in women and frequently produce overlapping head and follicle symptoms. For women experiencing both, evaluation should typically include a thyroid panel, ferritin level, hormone testing, and autoimmune screening.
What Is Cephalgia Alopecia?
Cephalgia alopecia is a rare headache disorder first described in a case report in 2006 and reviewed in detail in the 2020 Bedrin and Dougherty paper. It is defined as recurrent burning, stabbing pain in the head and neck that is followed by shedding in the corresponding region of the scalp.
The proposed mechanism, as described earlier, involves trigeminal and cervical nerve activation depleting substance P and CGRP at the follicle level. Researchers also suggest that cephalgia alopecia may share a disease spectrum with nummular headache accompanied by trophic skin changes.
Common signs include:
- Localized burning, stabbing, or pressing pain
- Shedding that appears in the exact area where pain is felt
- Recurrent episodes that follow a predictable pattern
The mainstay treatment for both the pain and the shedding is OnabotulinumtoxinA, commonly known by the brand name Botox. Diagnosis is typically made based on clinical history and a positive response to OnabotulinumtoxinA injections.
A grid-like injection technique used in nummular headache is being studied for cephalgia alopecia, and early evidence suggests it may relieve both symptoms simultaneously. As with any injection therapy, possible side effects include temporary injection site soreness, bruising, weakness in nearby muscles, and short-term head discomfort.
When to Seek Medical Advice
Consult a specialist if you experience:
- Sudden or unusual shedding patterns
- Persistent head pain affecting daily life
- Scalp tenderness, burning, or localized inflammation
- Symptoms that worsen over time or fail to improve with rest
Brief episodes tied to acute stress often resolve on their own, but repeated or escalating symptoms should be evaluated. Your doctor may examine the scalp closely, check for nerve sensitivity, and order targeted laboratory tests.
When both symptoms appear repeatedly or interfere with quality of life, early assessment can prevent long-term follicle damage and reveal underlying medical conditions that need treatment.
What Dr. Kopelman Looks For During Evaluation
At Kopelman Hair, Dr. Kopelman checks:
- Where the pain occurs and how often
- Patterns of shedding and follicle miniaturization
- Scalp condition, sensitivity, and medical history
- Possible connections to medications or recent illness
Diagnostic tests may include:
- Bloodwork for thyroid, ferritin, vitamin D, and hormone levels
- Autoimmune screening, including ANA and inflammatory markers
- Infectious disease testing such as RPR when clinically indicated
- Scalp analysis, pull tests, and stress evaluations
This combined approach helps pinpoint the exact cause and create a tailored treatment plan, often in collaboration with a neurologist or dermatologist when needed.
Comparing Symptoms by Cause
Comparing Symptoms by Cause
This table compares common pain types and shedding patterns linked to different possible causes.
Recognizing patterns helps you and your provider take targeted steps early.
Common Myths About Head Pain and Hair Shedding
Misinformation can lead to unnecessary worry. Here are a few common myths:
Focus on credible symptoms and seek medical input when in doubt.
Treatment Options for Headache and Hair Loss
The right treatment depends on what’s causing your symptoms.
For stress-related issues:
- Develop consistent sleep, hydration, and meal routines
- Try relaxation techniques such as deep breathing, progressive muscle relaxation, or mindfulness
- Consider acupuncture, yoga, or guided meditation as complementary approaches
Effective stress management can promote regrowth and ease overall discomfort.
For scalp conditions:
- Use antifungal or medicated shampoos as prescribed
- Treat infections early before they spread
- Avoid tight hairstyles and harsh chemical treatments
- Address underlying dermatologic conditions like seborrheic dermatitis
For autoimmune or hormonal causes:
- Manage hormones through appropriate medical care
- Consider corticosteroids for hair loss alopecia
- Use supplements only under medical supervision
- Coordinate care between dermatology, endocrinology, and rheumatology when needed
For cephalgia alopecia:
- OnabotulinumtoxinA (Botox) injections are the established treatment for both pain and shedding
- Diagnosis and treatment are typically managed by a neurologist familiar with the condition
- A grid-like injection technique adapted from nummular headache treatment is showing promise
For migraines and hair loss specifically:
- Standard migraine prevention, including triptans, beta-blockers, or CGRP inhibitors when appropriate
- Address co-occurring stress, sleep, and nutritional factors
- Monitor follicle response as migraine frequency decreases
For infectious causes:
- Targeted antimicrobial therapy when an infection is identified
- For neurosyphilis, intravenous penicillin G is the standard of care, with both head pain and shedding typically resolving within weeks of treatment
Understanding the common types of alopecia helps determine when a medical solution is needed or when lifestyle changes may be enough.
Frequently Asked Questions
Yes, in certain cases. Chronic or severe migraines can activate trigeminal and cervical nerves that innervate follicles, depleting growth-supporting neuropeptides. Patients with frequent migraines who notice patchy shedding in painful areas should be evaluated for cephalgia alopecia.
Some forms of alopecia, especially those linked to autoimmune disease like lupus or Hashimoto’s thyroiditis, can co-occur with chronic head pain. The shedding itself does not cause pain, but the underlying systemic condition often produces both symptoms.
Yes. Scarring alopecia, alopecia areata, and certain forms of folliculitis can mimic the appearance of cephalgia alopecia. A dermatologist can differentiate between them through scalp examination and, if needed, a biopsy.
As with any injection, OnabotulinumtoxinA carries possible side effects including injection site discomfort, bruising, temporary weakness in nearby muscles, and brief head discomfort. Working with a specialist experienced in this treatment minimizes these risks.
If head pain is your dominant symptom and shedding follows the pain in a specific region, start with a neurologist. If shedding is widespread and pain is mild or generalized, a hair restoration physician or dermatologist is a strong starting point. Many patients benefit from coordinated care between both specialists.
If you’re experiencing persistent head discomfort or unexplained shedding, don’t wait to find answers. Schedule a consultation with Dr. Kopelman at Kopelman Hair to receive a personalized evaluation and expert care tailored to your needs.